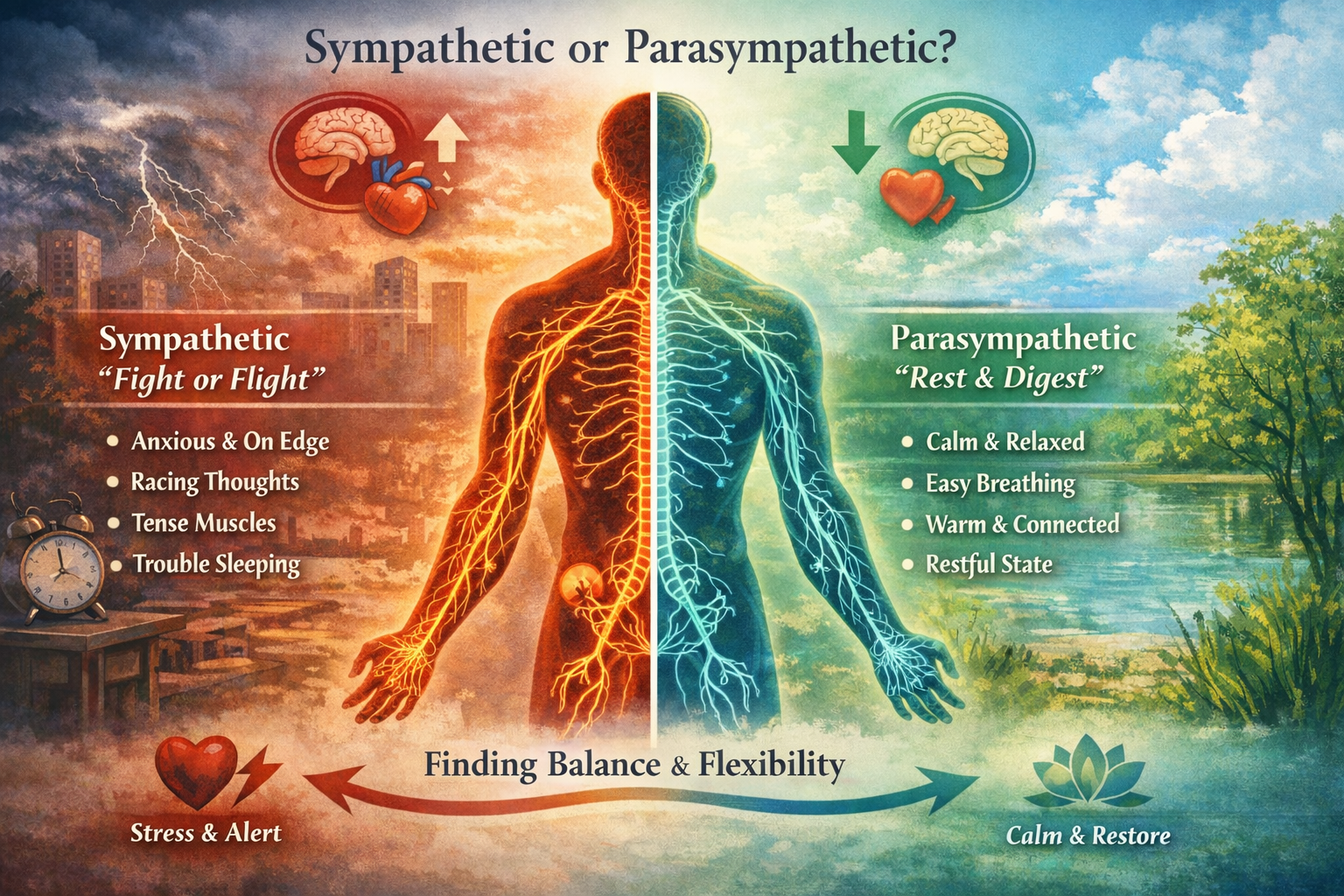
Sympathetic- vs. Parasympathetic-“Dominant”: Helpful shorthand, but not a diagnosis
Have you ever said—or thought—something like:
“I feel stuck in fight/flight all the time…”
“I just feel shut down and exhausted…”
At Time to Renew You LLC, we often hear this language because it feels right. But terms like “sympathetic dominance” and “parasympathetic dominance” are metaphors—not medical diagnoses. Your nervous system isn’t “one mode” forever. It’s constantly adjusting to what’s happening around you and inside you. The goal isn’t to be permanently in one state, but to flexibly shift between states as needed—and to recover well after stress.
Below, we’ll explore what these terms really mean, how your body is responding, and what the research says about stress, arousal, and calm regulation—written especially for therapy clients.
What the Nervous System Actually Does
Your autonomic nervous system (ANS) has two major branches:
Sympathetic Nervous System (SNS): mobilizes energy, gets you ready to face threats (fight/flight).
Parasympathetic Nervous System (PNS): supports rest, digestion, connection, and recovery.
Research now emphasizes that these systems rarely “dominate” in isolation. Instead, they work together in patterns of activation, recovery, and flexibility. Healthy functioning is about the balance and adaptability between them—not a permanent state of dominance. (Waxenbaum, Reddy, & Varacallo, 2023; Weissman et al., 2021)
What “Sympathetic-Lean” Really Looks Like
People often use “sympathetic dominance” to describe a sense of being chronically activated or “on alert.” This pattern usually arises when your body stays in a protective mode for too long.
Common experiences include:
Feeling on edge, tense, or easily startled
Racing thoughts or irritability
Difficulty settling your body or mind
Shallow breathing or muscle tension
Trouble sleeping or falling asleep
Digestive upset at stressful moments
These responses make sense: your SNS prepares you to deal with challenge. The issue arises when your body can’t turn off that alert state effectively.
The American Psychological Association describes how chronic stress keeps your body in a mode of alertness that impacts mood, muscles, digestion, sleep, and overall wellbeing. (American Psychological Association, 2018)
What “Parasympathetic-Lean” Really Looks Like
On the flip side, people sometimes describe feeling “shut down” or drained as being “parasympathetic dominant.” But research warns that this kind of collapse often reflects exhaustion or overwhelm—not a restful, regulated PNS state.
True parasympathetic activation feels like:
Calm alertness
Ease in your body
Comfortable breathing and warmth
Engagement and safety in social connection
In contrast, shutdown may include:
Heavy fatigue
Difficulty initiating tasks
Feeling disconnected or numb
Slowed thinking or motivation
These kinds of shutdown responses can show up after chronic stress, trauma, or burnout—not because you’re naturally “PNS dominant,” but because your system needs restoration and regulation support.
How Professionals Think About Autonomic Patterns
Rather than labeling someone as “dominant” in one system, clinicians and researchers assess:
1. Reactivity
How strongly your body responds to stressors.
2. Recovery
How quickly your system returns to baseline after stress.
3. Flexibility
How smoothly you shift between activation and rest based on context.
One commonly studied marker is heart rate variability (HRV)—a measure of how your heart rate naturally fluctuates with breathing and regulation. Higher HRV is generally linked with better regulation and resilience; lower HRV tends to show up with chronic stress or dysregulation (Olivieri et al., 2024; Besson et al., 2025). But HRV is not a diagnosis—it’s a tool that can be helpful when tracked over time.
What This Means for You
Labeling your system as “sympathetic” or “parasympathetic dominant” can feel validating—but the real goal is to notice patterns and support shifts toward balance, flexibility, and recovery.
Here’s what research suggests helps nervous systems become more regulated:
Foundational supports
Consistent sleep (timing matters)
Movement you enjoy, regularly
Balanced nutrition and hydration
Reducing avoidable stressors (like excess caffeine or poor sleep habits)
Skills that support nervous system regulation
Slow exhale breathing
Mindful awareness practices
Safe social connection
Grounding activities (nature, rhythm)
These are not quick “switches,” but practices that strengthen your ability to shift gradually over time.
When to Seek Extra Support
If your stress responses are interfering with daily functioning—such as persistent panic, chronic fatigue, overwhelming anxiety, or physical symptoms like fainting or palpitations—it’s important to talk with a clinician. Autonomic patterns can be influenced by medical, psychological, and emotional factors.
Therapy at Time to Renew You LLC can help you understand your patterns in a safe, compassionate, and research-informed way, and develop skills that support resilience and regulation.
References (APA 7)
American Psychological Association. (2018, November 1). Stress effects on the body. https://www.apa.org/topics/stress/body
Besson, C., et al. (2025). Assessing the clinical reliability of short-term heart rate variability measurements in various settings and positions. Scientific Reports. https://www.nature.com/articles/s41598-025-89892-3
Olivieri, F., et al. (2024). Heart rate variability and autonomic nervous system imbalance in aging: A biomarker perspective. Ageing Research Reviews. https://www.sciencedirect.com/science/article/pii/S1568163724003398
Waxenbaum, J. A., Reddy, V., & Varacallo, M. (2023). Anatomy, autonomic nervous system. In StatPearls. StatPearls Publishing. https://www.ncbi.nlm.nih.gov/books/NBK539845/
Weissman, D. G., et al. (2021). Correlation of sympathetic and parasympathetic nervous system activity during emotional and cognitive challenges. Autonomic Neuroscience: Basic and Clinical. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7987796/